
Maternal and child health inequities have persisted in the United States (U.S.) for decades despite having one of the most advanced healthcare systems in the world [1]. The root causes of these inequities are multifaceted but include factors such as deep seated social divisions [2], socio-ecological indicators like wealth disparities and the built environment [3], as well as limited access to care in rural areas [4]. These root causes, also known as the social drivers of health (SDOH), account for up to 80% of health outcomes [5]. Defined by the World Health Organization (WHO) as “the conditions in which people are born, grow, work, live, and age” ([6] p1), individuals experiencing these environmental drivers (e.g., living in a food desert) may result in the presence of non-medical, health-related needs (e.g. food insecurity). It follows then that improving maternal and child health outcomes must include addressing non-medical needs as standard of care.
Technology-enabled, closed-loop referral networks have emerged as one promising digital tool to increase access to community resources, address non-medical needs, and improve health outcomes [7, 8]. The foundational theory behind digital closed-loop referral networks is a socioecological framework that recognizes the interconnected layers influencing our health: policy, institutions, community, relationships and individual-level factors [9]; and seeks to overlay these with technical infrastructure to produce a digital care continuum.
This focus on a care continuum is critical given that health and community care delivery is highly fragmented, placing a significant burden on individuals to self-navigate complex systems to meet their needs [10]. “Closing the loop” infers that the resulting referral network is not a one-way system, but rather a person-centered community of care that values and captures outcomes delivered through engaged community partners. This allows technology-enabled closed-loop referral networks to answer not only whether an individual was connected to services, but also whether their needs were ultimately resolved [11].
Moving from a maze of resources to a coordinated system of care
First 1,000 Days Suncoast is a tri-county initiative in southwest Florida that was started in 2018 by the Charles & Margery Barancik Foundation, Sarasota Memorial, and other stakeholders [12]. What started with 32 partner organizations has now grown to more than 95 community partners addressing the needs of families with young children [12]. The initiative connects healthcare providers and nonprofit organizations to reduce systemic barriers to care and improve outcomes for new parents and their children.
A critical construct of First 1,000 Days was to move from a “maze of resources” to a streamlined and coordinated system of care (Fig. 1) [12,13,14]. In 2020, the initiative partnered with Unite Us, a healthcare technology company specializing in closed-loop referral platforms, to provide the technical infrastructure needed to fulfill the initiative’s vision. This tool has been critical in understanding the needs of the community and provides an efficient care pathway for patients with non-medical needs, giving mental health and healthcare providers the confidence to implement universal SDOH screening with a tool for taking action when needs are identified.
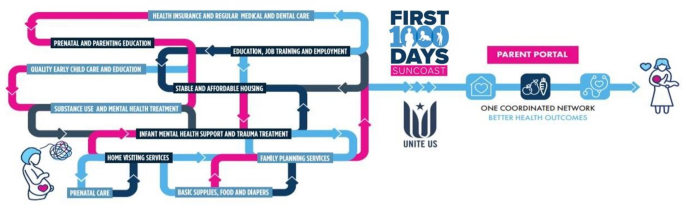
First 1,000 Days Suncoast Theory of Change Infographic
Following the Collective Impact Model, Sarasota Memorial serves as the backbone organization for First 1,000 Days Suncoast. As the safety net hospital system for Sarasota and surrounding counties, it provides care to a significant number of low-income and underserved pregnant patients. Sarasota Memorial is one of the largest public community health care systems in the state of Florida, including two hospitals, urgent care centers, and a free-standing Emergency Care Center. It has nationally recognized level 3 maternity obstetrical services with a level 3 NICU. It is Joint Commission accredited and Magnet and Baby Friendly designated. In August 2020, as part of the First 1,000 Days initiative, Sarasota Memorial incorporated the Unite Us closed-loop technology into its obstetric care units to ensure new parents with non-medical needs were referred to First 1,000 Days’ community partners upon discharge.
The purpose of this study was to determine whether the implementation of the Unite Us platform at Sarasota Memorial between August 27, 2020, and January 31, 2023, reduced all-cause and OB-related healthcare resource utilization (HCRU) up to six months postpartum for patients with a live birth and one or more care referrals through Unite Us, when compared with those who had a live birth at the hospital prior to implementation.
link





