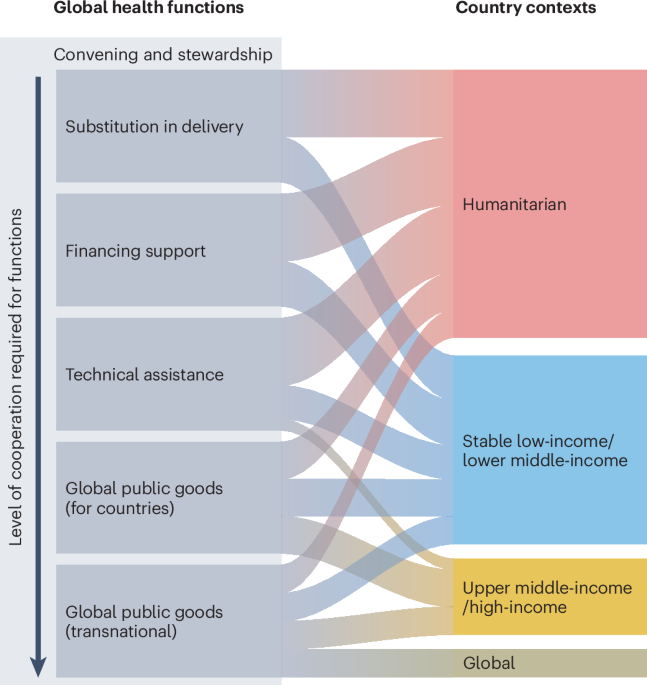
In Fig. 1, we present a non-exhaustive set of functions and contexts for the global health system, building on previous frameworks3,4. The functions are presented in a continuum for collaboration, starting with substitution in delivery (where external actors fund, contract and oversee execution in countries of key functions such as health service delivery, strategy and policy development, and data monitoring), which represents the lowest level of country ownership and leadership.
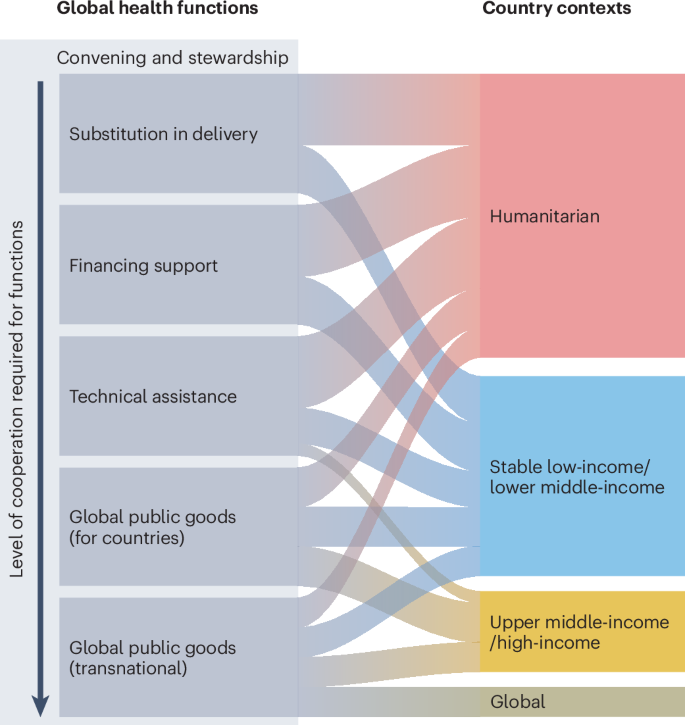
Functions and contexts for global health.
We identify four broad contexts to apply these functions: humanitarian settings; stable low-income and lower-middle income countries (LLMICs; conflict-free with a state able to exercise authority over the whole country); upper middle-income countries (UMICs) and high-income countries (HICs); and the global, trans- and international setting. Across these contexts, marginalized population groups within countries must not be forgotten. Below, we use this framework to question what functions are still relevant for global health and which should be emphasized in each context.
Substitution for, or even crowding out, country functions, with limited engagement with and oversight by the state, must be avoided. One of the partial contributions of global health over recent decades is substantial increases in public health capacity in LLMICs. However, the current global health financing crisis reveals how much de facto substitution has been occurring in contexts where it should not. Stop orders decided in a donor country one day translate to health workers not going to work and patients not receiving life-saving treatments the next5.
Yet, there is still a plausible need for substitution in humanitarian settings (such as war and conflict zones), and more arguably in the lowest resource and capacity contexts, where the state does not have effective jurisdiction nor capacity to deliver, and where people experience the worst health. Substitution is also relevant for marginalized populations explicitly or implicitly excluded from the systems overseen by national and subnational governments. And yet, even where substitution might be justified, it should be seen as a temporary mode rather than a permanent commitment, with active efforts to revert to local ownership and delivery by the state as soon as possible. Substitution in stable LLMICs is not warranted or sustainable, and the current crisis is an opportunity to resolve this.
Financing support and direct technical assistance to countries will likely have a smaller role in this new era with substantially lower levels of health aid. Most financial resources for health in most countries are already mobilized domestically, and this will need to be expanded6. Technical assistance will be disrupted by the smaller footprint of aid ecosystems from vendors in HICs and of multilateral agencies who provide such assistance. But financing and technical support will remain important for humanitarian settings and for most low-income and many lower-middle income countries.
There is a strong case to sustain technical assistance even when major financing support has ceased in these settings. However, there are important questions about how grants and concessional loan channels can be aligned to country budgets and who and how to deliver technical assistance that genuinely and sustainably strengthens health systems at country level. The value and efficiency of technical assistance, the drive for ‘localization’ of such assistance to be delivered through national and local institutions, and the potential greater value of ‘South–South’ technical exchange need more reflection.
Global (or regional) public goods have been championed as the most important function of the global health system4,7, even if in practice and funding they have been eclipsed by financing support and technical assistance to countries. Global public goods can be differentiated between goods to be directly applied by and within countries — such as research, knowledge sharing, guidance, norms, standards, data and monitoring, market shaping and procurement — and goods for international collaboration to address transnational threats such as surveillance of infectious diseases, infectious disease control efforts and international legal instruments.
These supranational public goods must meet the demands of countries and provide added value, especially in an era of artificial intelligence where knowledge does not solely spring from a single authoritative source. Important discussions are needed on how to generate these global public goods through collective action, collaborative processes and fair contributions (avoiding ‘free riders’), and to clarify the role of regional versus global institutions.
Underpinning all these functions are the convening and stewardship processes of global health to support exchange between actors and countries, collaboration and decision-making, occurring at different levels of governance and supported by an array of organizations. The geopolitical changes that continue to unfold rapidly question what stewardship of global health, and its processes, should look like after 2030.
link







