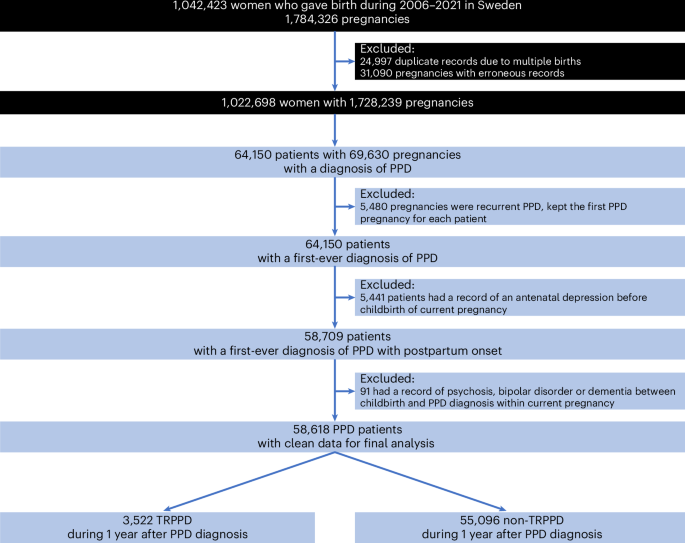
In this large, population-based cohort of patients with first-ever diagnosed PPD, we found the occurrence of treatment resistance to be common in patients with PPD. Moreover, our study pinpoints that multiple demographic and clinical profiles, including lower educational level, lower income, cigarette smoking, primiparity, cesarean section, preterm delivery (32–36 weeks) and pre-existing physical and psychiatric conditions, are independently associated with a higher risk of developing TRPPD.
In this study, the proportion of patients with PPD who fulfilled the predefined TRPPD was 6.0%. Even with stricter criteria applied in our study, the proportion of treatment resistance was higher than the proportion reported in a previous study conducted in the United States22. However, the numbers of peripartum depression (2.5%) and treatment resistance (5.0%) in the US study might have been underestimated because the study included only insured people and excluded women with prior psychosis, bipolar disorder or dementia22. By contrast, the proportion of treatment resistance in our study was lower than that reported among patients with non-perinatal depression in population-based studies in Sweden12 (13%) and Denmark7 (15%), and even lower than the proportions reported in clinical trials10 (30%). Several factors may explain the lower treatment resistance in PPD compared with non-perinatal depression. First, compared with patients with non-perinatal depression, some patients with PPD may hesitate to continue or initiate pharmacotherapy or choose psychotherapy over pharmacotherapy due to concerns of potential harmful effects on the infant through breastfeeding6; therefore, PPD patients may receive less pharmacotherapy during the study period. Indeed, our data showed that 13.5% of patients did not receive any pharmacological or ECT/rTMS treatment during the postpartum year. Thus, the low proportion might indicate that women with PPD are somewhat untreated or undertreated, which is supportive in previous reports6,23. Second, in 2010, a screening for PPD was introduced in Swedish national guidelines. Therefore, patients diagnosed from 2010 onward might have less severe symptoms; and timely treatments/interventions which, if successful, may contribute to the lower treatment resistance in our study. Our results indicate lower risks of TRPPD in patients diagnosed after 2010 than before 2010, which also supports this explanation. In addition, compared with previous studies in which patients were ascertained through inpatient/outpatient care diagnosis7,12, our study including primary care diagnosis may have captured more mild or moderate cases, leading to lower treatment resistance.
We found that several demographic factors, including lower educational attainment or household income, being non-cohabiting, being born outside Sweden and living in northern Sweden, were associated with higher risk of TRPPD. One potential interpretation is that socioeconomically disadvantaged patients may have less accessibility to healthcare resources and social support, resulting in deteriorating disease severity and treatment response. Similar findings have been observed for non-perinatal depression in previous studies24. For example, Gronemann et al.25 found that patients with depression becoming unemployed were at higher risk of treatment resistance. In addition, substantial evidence has indicated that low socioeconomic status was associated with elevated levels of depressive symptoms26,27, which also supports our findings.
Moreover, the results of higher risk of TRPPD among patients who were smoking is in line with findings in people with non-perinatal depression24. Possibly, smoking individuals have more severe depressive symptoms28, or smokers may receive bupropion for smoking cessation29; thus, they might receive more antidepressants while not being depressed. Besides, smoking is considered an indicator of unfavorable socioeconomic status in the Swedish female population30. These factors may explain the higher risk of TRPPD among smoking patients. It is also possible that smoking may interact with drug metabolism and affect treatment effect31, leading to more antidepressant treatments.
Although some studies indicate that multiparity may predict prolonged depressive symptoms19, most studies indicate that multiparity is associated with lower risk of PPD32. By contrast, in our data, PPD patients with two births (the most common type in Sweden) had a lower risk of TRPPD but not among patients with three or more births. However, in the sensitivity analysis excluding patients with prior psychiatric disorders, as well as in the mutually adjusted analysis, a higher risk of TRPPD was observed only among patients with three or more births. Thus, more research is needed to corroborate our findings on the link between parity and TRPPD. In addition, PPD patients who gave birth through cesarean section were more likely to develop PPD33. Cesarean section, particularly acute cesarean section, can lead to a negative delivery experience20, which may drive these patients to more severe symptoms of postpartum depression21. Preterm delivery at 32–36 weeks was associated with a higher risk of TRPPD. It is plausible that preterm birth entails higher risk of neonatal complications and stressful experiences such as admission to neonatal intensive care units34, which may contribute to worse prognosis of PPD. However, very preterm birth (22–31 weeks) was not associated with TRPPD, which argues against such explanation. In addition, low birth weight, another risk factor for neonatal complications, was not associated with TRPPD. We did not note a material difference in treatment response between patients with a live birth and those with a stillbirth, although the etiology of PPD may differ between these two groups, as depression following a stillbirth may be more closely related to grief over the loss.
Our finding on the higher risk of TRPPD among patients with previous physical conditions is also in line with studies on non-perinatal depression15,35. This could be attributed to the chronic inflammation, or altered hepatic or renal functions, or drug interactions with antidepressant due to these physical comorbidities31. Recent findings indicate non-responders to antidepressant treatment have higher inflammatory levels compared with responders36. Of note, we did not observe a higher risk of TRPPD among patients with gestational diabetes or pre-eclampsia, although mothers with such conditions generally have a higher rate of PPD32,37.
Pre-existing psychiatric conditions have been repeatedly and consistently associated with increased risk of treatment resistance in patients with non-perinatal depression15,38. In the study by Cepeda et al.22, women with perinatal depression who developed treatment resistance had higher rates of psychiatric comorbidities in the previous year than those who did not develop treatment resistance. However, the result is from descriptive comparisons without confounding adjustment22. In this study, we illustrated that pre-existing psychiatric conditions, both any psychiatric disorder and a range of specific psychiatric disorders, were associated with a higher risk of TRPPD. Patients with pre-existing psychiatric conditions might have received antidepressants to treat depression or conditions other than depression, and therefore could have become somewhat tolerant to antidepressants intended for their PPD39. By contrast, patients with prior premenstrual disorders were at a lower risk of TRPPD. This subgroup of patients are sensitive to normal changes of gonadal steroid levels40 and may represent a ‘hormone-sensitive’ phenotype of PPD17. Theoretically, in this subgroup, depressive symptoms are triggered by the normal drop of gonadal hormones after delivery, but symptoms may remit when hormone levels begin rising again. Future studies, however, are needed to elucidate the role of hormonal factors in treatment response of PPD. It is worth noting that when patients with a psychiatric history were excluded, we saw similar results for risk factors, including socioeconomic status, parity and prior physical comorbidities. This suggests these risk factors are independent of prior psychiatric conditions.
Of note, we found that most factors associated with TRPPD in our study overlap with the psychosocial risk factors for PPD. A probable explanation could be that PPD patients with these factors are more likely to develop more severe depression or require more intensive treatment due to pre-existing mental conditions, which increases their chances of developing treatment resistance or being classified as treatment resistant.
Several strengths of our study assure robustness of our findings. The nationwide population-based sample together with high-quality, prospectively collected healthcare register data enabled a representative sample of treatment resistance among women with PPD and a comprehensive assessment of various risk factors for TRPPD. Our study has weaknesses. First, in Sweden, depression is often managed in primary care41. While we used antidepressant prescriptions for identification, we might have missed mild PPD cases who were not prescribed pharmacotherapy as we only had primary care data from five counties. Yet this concern was addressed by the almost identical results when repeating the analysis using data from only these counties. Second, psychotherapy is the first-line treatment for mild to moderate depression in Sweden. However, due to lacking information on psychotherapy, the influence of psychotherapy on treatment response was not considered in our study. Future studies incorporating both psychotherapy and pharmacotherapy are highly warranted. Third, we may have some degree of misclassification of treatment resistance as our definition did not consider the dose of treatment. However, largely comparable results were obtained when utilizing two alternative definitions of treatment resistance. In addition, misclassification of treatment resistance may occur among patients with prior psychiatric disorders as these patients could restart or continue treatments for their prior illness during the postpartum period, leading to overestimation of TRPPD. The concern, however, was partially alleviated as we obtained similar results when excluding PPD patients who had any pre-existing psychiatric conditions. Last, our results might not be generalized to populations outside Sweden where different healthcare service systems apply.
In conclusion, based on a nationwide sample, our study shows that the prevalence of treatment resistance was common in patients with PPD. We found primiparous patients with lower socioeconomic status, cigarette smoking and pre-existing physical and psychiatric conditions are at a higher risk of developing treatment resistance. These findings may provide grounds for practical risk assessment at PPD diagnosis and highlight the need for personalized management strategies (for example, actively monitoring treatment response to aid earlier medication adjustments), particularly for patients identified as at risk for worse prognosis.
link





